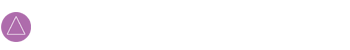This guide explains where people can get tested and what typically happens before, during, and after a sleep study.
Where can they get a sleep study in Melbourne?
A Sleep Study Melbourne pathway usually allows patients to get tested through a hospital sleep unit, a private sleep clinic, or a home sleep test arranged by a sleep physician or GP referral pathway. The “best” option depends on symptoms, budget, and whether complex monitoring is needed.
Many people start by speaking with a GP, who can refer them to a sleep specialist or directly to a service that offers testing.
Should they choose an in clinic sleep study or a home sleep test?
They generally choose an in clinic study when symptoms are complicated, safety monitoring is important, or previous tests were inconclusive. They often choose a home sleep test when obstructive sleep apnoea is strongly suspected and a simpler setup is appropriate.
Home testing can be more comfortable and accessible, but it may not capture as many signals as an overnight lab study.
What conditions can a sleep study help diagnose?
A sleep study commonly helps diagnose obstructive sleep apnoea, central sleep apnoea, snoring related breathing issues, and oxygen drops overnight. In more detailed in clinic studies, it can also assess limb movements, unusual night behaviours, and sleep stage disruptions.
If daytime sleepiness is severe, the clinician may also consider additional daytime testing.
How do they book a sleep study in Melbourne?
They typically book by first discussing symptoms with a GP, who may arrange a referral to a sleep physician or a sleep clinic. The clinic then reviews symptoms and medical history and recommends either a home test or an in lab polysomnography.
Some providers also allow self enquiry, but a clinician is usually involved to ensure the correct test is selected.
What happens before the sleep study appointment?
They are usually asked about sleep habits, medications, alcohol intake, work schedule, and symptoms such as snoring, choking, headaches, reflux, or restless legs. They may be given instructions such as avoiding caffeine late in the day and keeping their routine as normal as possible.
If it is a home test, they are often shown how to fit the sensors or given printed instructions.
What happens during an in clinic sleep study?
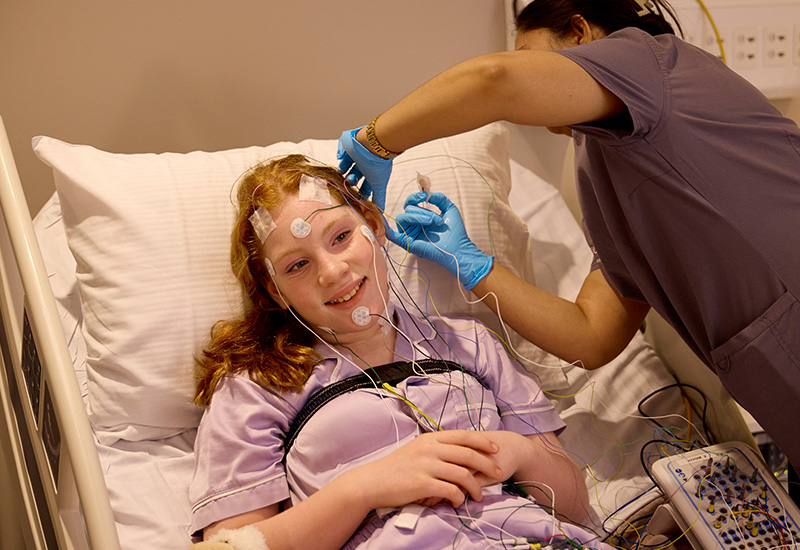
They arrive in the evening, settle into a private room, and a technician applies sensors to measure breathing, oxygen levels, heart rate, brain activity, eye movements, and muscle tone. This is designed to track both sleep stages and breathing events through the night.
Most people can move and turn in bed, even with the wires attached, and staff monitor the signals from another room.
What happens during a home sleep study?
They take the equipment home and attach a small set of sensors, commonly including a breathing effort belt, a nasal cannula for airflow, and a finger probe for oxygen. Some systems also measure body position and snoring.
They sleep in their own bed, return the device the next day, and the recorded data is analysed by trained staff.
Will they be able to sleep normally with the sensors on?
They may sleep a little differently at first, especially in a clinic environment, but the study can still capture enough information to be useful. Technicians expect some disruption and focus on collecting clear signals across the night.
If the person wakes often, the clinician can still interpret patterns in breathing, oxygen, and arousals.
What is CPAP titration and when does it happen?
CPAP titration is when air pressure is adjusted during sleep to find settings that prevent apnoeas and oxygen drops. It may be done on a separate night or during a split night study, depending on what the clinician orders and how quickly severe sleep apnoea is identified.
Not everyone needs titration, but it is common when moderate to severe obstructive sleep apnoea is found.
What happens after the sleep study in Melbourne?
They usually receive a follow up appointment to explain results, including measures like the Apnoea Hypopnoea Index and oxygen saturation trends. The clinician then recommends a plan, which may include CPAP, a mandibular advancement device, weight management support, positional therapy, or further testing.
If symptoms do not match the results, the clinician may adjust the approach rather than relying on a single test alone.
How long does it take to get results?
Results timing varies by provider, but many services deliver a report within days to a couple of weeks. Urgent cases may be prioritised, especially if oxygen drops are significant or daytime sleepiness is creating safety risks.
They can ask the clinic upfront about reporting timeframes and follow up availability.
What should they bring or do on the night?
For an in clinic study, they typically bring comfortable sleepwear, toiletries, and any usual nighttime medications. They should follow the clinic’s guidance about caffeine, alcohol, and naps, since these can change sleep quality and breathing patterns.
They can also mention any anxiety about the setup, because technicians can often make simple adjustments to improve comfort.
How do they choose a good sleep study provider in Melbourne?
They can look for a provider that offers clear clinical oversight, explains which test is being used and why, and provides timely follow up to discuss treatment options. It also helps if the service can support the full pathway, from testing to CPAP trials or alternative therapies.
If costs matter, they can ask for an itemised estimate and whether Medicare or private health rebates may apply.
FAQs (Frequently Asked Questions)
Where can I get a sleep study done in Melbourne?
In Melbourne, you can get a sleep study through hospital sleep units, private sleep clinics, or via home sleep tests arranged by a sleep physician or through GP referrals. The best option depends on your symptoms, budget, and whether complex monitoring is needed.
Should I choose an in-clinic sleep study or a home sleep test?
An in-clinic sleep study is recommended if your symptoms are complicated, require safety monitoring, or if previous tests were inconclusive. A home sleep test is suitable when obstructive sleep apnoea is strongly suspected and a simpler setup suffices. Home testing offers more comfort and accessibility but may not capture as many signals as an overnight lab study.
What conditions can a sleep study diagnose?
Sleep studies commonly help diagnose obstructive and central sleep apnoea, snoring-related breathing issues, and oxygen drops during the night. Detailed in-clinic studies can also assess limb movements, unusual night behaviours, and disruptions in sleep stages. Additional daytime testing may be considered if severe daytime sleepiness is present.
How do I book a sleep study in Melbourne?
You typically start by discussing your symptoms with a GP who may refer you to a sleep physician or directly to a sleep clinic. The clinic will review your symptoms and medical history to recommend either a home test or an in-lab polysomnography. Some providers allow self-enquiry but clinician involvement ensures the correct test selection. See how to choose the right provider for sleep testing Adelaide.
What should I expect before and during the sleep study?
Before the appointment, you’ll be asked about your sleep habits, medications, alcohol intake, work schedule, and symptoms like snoring or restless legs. Instructions may include avoiding caffeine late in the day and maintaining your usual routine. During an in-clinic study, sensors will be applied to monitor breathing, heart rate, brain activity, and more while you sleep overnight. For home tests, you’ll be shown how to attach sensors yourself and will return the device after sleeping at home.
What happens after my sleep study in Melbourne?
After the study, you’ll usually have a follow-up appointment to discuss results such as the Apnoea Hypopnoea Index and oxygen saturation trends. Based on findings, the clinician may recommend treatments like CPAP therapy, mandibular advancement devices, weight management support, positional therapy, or further testing. Treatment plans are tailored especially if symptoms do not align perfectly with test results.